A recent publication by a renowned molecular biologist sparks a media frenzy surrounding resistance.
Doctor Shinji Kasai is somewhat of hero within the mosquito community. Dr. Kasai is a molecular biologist who has devoted his entire career and much of his life to research into the genetics of insecticide resistance in mosquitoes. His work primarily focuses on understanding the mechanisms of resistance as a means for developing strategies to overcome it.
In June 2014, he released a much-publicized paper on the combined effects of three knockdown resistance (kdr) mutations in Aedes aegypti. The paper has since become a foundational work for field scientists battling resistance around the world. Kasai and his team were the first to demonstrate a causal relationship between specific genes and pyrethroid sensitivity in mosquitoes. Using frog oocytes with the resistance mutations built in, Kasai was able to show that the mutations altered how sodium channels communicate and, in turn, the levels of resistance those mutations conferred. The study also demonstrated that co-occurrence of all three alleles (one of two or more alternative forms of a gene that arise by mutation and are found at the same place on a chromosome) resulted in resistance 11x higher than two alone.1
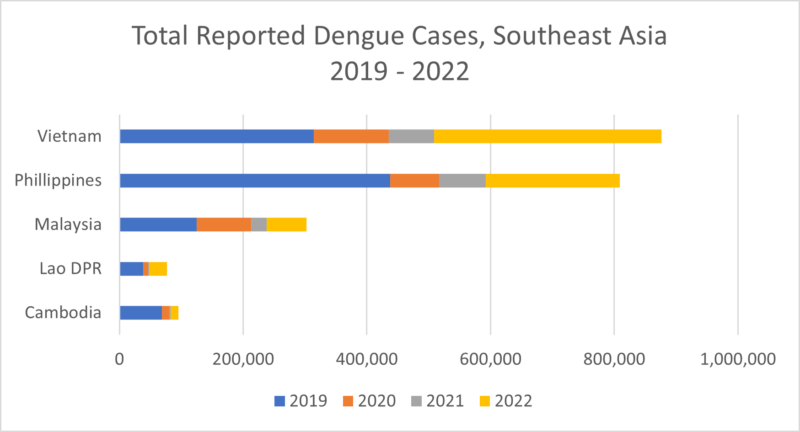
Source: WHO Dengue Situation Updates 610-662
The mutations in question act by substituting for wild type alleles, preventing pyrethroid insecticides from binding properly at their Voltage-Gated Sodium Channel (VGSC) target sites. VGSCs are the basic ion channels crucial for the resting potential and action potentials in neurons. Proving the causal relationship was a significant breakthrough in the field of genetics and the study of insecticide resistance in mosquitoes. It has enabled mosquito entomologists to improve their understanding of how resistance to insecticides evolves and has opened the way for the development of new strategies for controlling mosquito populations and reducing the spread of diseases.
Front Page News
Dengue is just one arbovirus in a region where mosquito-borne illnesses are common. The tropical climate and packed urban centers of the Mekong subregion are ideal for container mosquitoes such as Aedes aegypti. For his part, the prolific Kasai has published numerous discoveries over the past 15 years relating to resistance to conventional insecticides and pyrethroids in A. aegypti and other insects.
On December 21, 2022, Kasai’s newest paper was published in the medical journal Science Advances. The title of the paper included the phrase “super-insecticide-resistant dengue mosquitoes,” which created a firestorm in the mainstream media. The Washington Post published a piece on the paper and a number of smaller media outlets followed, providing a basic definition of resistance and along with bits from the paper.
Kasai’s study came on the heels of work by Boyer et al., published just months before, in January, 2022. Using the WHO diagnostic method, Boyer reported a resistant population of Ae. aegypti in Phnom Phen, Cambodia with mortality to pyrethrin and deltamethrin of 0 and less than 10% respectively. With this knowledge, Kasai again focused mainly in the Southeast Asia and on the co-occurrence of the kdr mutations that confer pyrethroid resistance there. The results were levels of resistance never been seen before in field populations of mosquitoes, as well as the unexpected appearance of a previously unremarkable allele, L982W, as being dominant among the resistant populations studied.
“Strains having these alleles exhibited substantially higher levels of pyrethroid resistance than any other field population ever reported.”
Shinji Kasai, National Institute of Infectious Diseases, Tokyo 2022
The work got underway as part of a larger study being conducted to assess pyrethroid susceptibility among world Aedes mosquito populations. For the study, Kasai’s team collected 23 wild mosquito populations captured from four countries: Vietnam, Indonesia, Ghana, and Taiwan.3 Kasai began by testing the resistance level of each population, then genotyping each for three well known VGSC mutations S989F, V1016c, F1534C, the same mutations he had investigated in his 2014 paper.
Kasai began by established a baseline lethal dose of permethrin using a susceptible population of mosquitoes in the lab. Two topical doses of 5.9 nanograms of permethrin were enough to cause mortality in 100% of a susceptible strain of Ae. albopictus mosquitoes. Next, Kasai evaluated this dose against the 23 wild populations. The results were sobering.
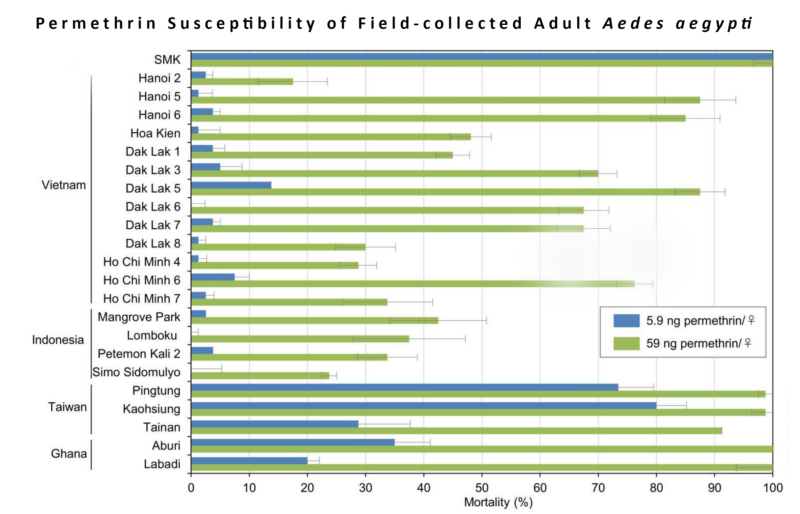
Permethrin resistance was so well established in the region, only four of the 23 wild mosquito populations demonstrated a mortality higher than 20% at the baseline dose. Next, Kasai and his team raised the dose by 10x and exposed the same populations to two topical doses of 59 ng of permethrin. Still, only two populations suffered 100% mortality. Two other populations – the populations of Hanoi 2 (Vietnam) and Simo Simulium (Indonesia) – showed mortality of less than 30% at 11x dose rate.
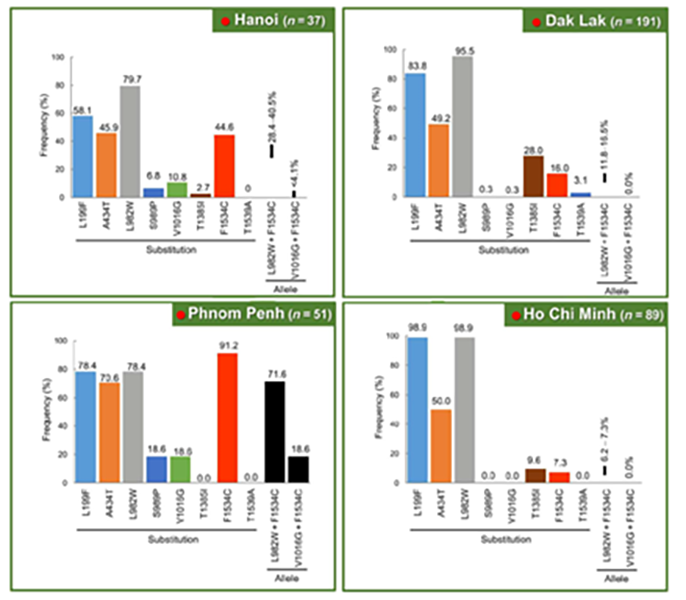
Kasai’s team then began a deeper investigation into two Vietnamese populations (Hanoi 2 and Hao Kien) to learn more about their genetic makeup. In that process, Kasai’s team unexpectedly found that 73.1 % of the Hao Kein population had an additional known substitution named L928W. Moreover, 41 of the surviving 42 mosquitoes (97.6%) from this population were L982W homozygotes – meaning that both parents had carried the L982W mutation.
Continuing Story
Sébastien Marcombe is a Ph.D. medical entomologist living in Lao People’s Democratic Republic (Laos). He is one of the region’s foremost experts on dengue and insecticide resistance in Ae. aegypti, and has been working in Laos since 2013. Marcombe is currently working as a medical entomological consultant for the World Health Organization (WHO) in Laos on its national malaria and dengue control programs.
Marcombe follows Kasai’s work closely. He says that identification of the L928W allele as a causal factor in these highly resistant populations will be important in helping shape future resistance fighting strategies. At the same time, Marcombe fears that the media attention may have been too narrowly focused on a single study, perhaps losing sight of the longstanding and pervasive problem that is pyrethroid resistance within the region.
Resistance has had a significant impact on mosquito control efforts across Southeast Asia. Since mosquitoes there are known to be resistant to a broad range of insecticides, it more difficult to effectively control mosquito populations and reduce the spread of important diseases such as dengue and malaria. Dichlorodiphenyltrichloroethane (DDT) had been used in the region to control mosquitoes until 1987, then the pyrethroid permethrin was introduced. Another pyrethroid, deltamethrin, was introduced in 2000. Pyrethroids have been used almost exclusively as adulticides since that time.
“It is good that the media picked up the story about Kasai’s study,” Marcombe says, “but what might have gotten lost is that resistance is already a big problem. It was a big problem before the discovery of L928W. It isn’t just something we need to watch out for in the future, it is a big problem now.”
Marcombe was a contributing author on the Boyer paper and has been experiencing the resistance challenge first-hand.
“From a high level, the results in the Kasai paper were consistent with what we’ve been seeing on Ae. aegypti in our lab for years. High levels of pyrethroid resistance are severely limiting our ability to control mosquitoes that spread disease. It is what you would expect to happen when your tools are limited, and you have to apply the same materials over and over again.”
There are other factors contributing to the onset of resistance as well. One of the cardinal rules in adulticiding, for example, is to provide complete coverage of the space that covers the flight range of the target mosquitoes. That rule is rarely adhered to in this region, where operators are more prone to make spot treatments around schools and other public buildings. The incomplete coverage that results contributes to the onset of resistance by exposing adult mosquitoes to sublethal doses of insecticide.
Similarly, Marcombe says many operators in the region are working with outdated equipment, which, when improperly calibrated, can also expose mosquitoes to sublethal doses. Another factor is that integrated vector management (IVM) programs in Southeast Asia are still the exception rather than the norm. Many mosquito control districts in the region lack the staff necessary to properly conduct mosquito surveillance – to be proactive rather than reactive. He says over-reliance on adulticides is another philosophical remnant left over from the DDT days.
“Dr. Kasai’s research is exceptional science,” Marcombe concludes. “Perhaps his work will bring some much-needed attention to what we are dealing with here. We need more people and better trained people. And we need new tools for this fight.”
*References can be found here.