Centers for Disease Control and Prevention
How Your Plate Affects Your Planet
Humanity’s growing demand for animal meat is driving a planetary crisis, accelerating climate change, devastating ecosystems, and threatening public health.
Two grim, almost surreal, 26-story buildings tower over the southern outskirts of Enzhou, about 500 miles west of Shanghai in China’s Hubei province. No one would mistake them for apartment complexes despite their neat grid of window-like slots. Indeed, their main inhabitants are not human at all. The buildings are designed specifically to meet the biological and reproductive needs of 600,000 pigs each. Here they will be bred, farrowed, fattened, and finally slaughtered to meet the exploding animal protein needs of China, which consumes half the world’s pork and is also its biggest pork producer.
It is the world’s largest vertical pig farm, designed to manufacture 54,000 tonnes of pork every year. The building’s design reflects its unique function. Each of its six giant elevators can hoist a load of 10 tons, or about 100 pigs, at a time. Every utility and process, from the building’s water supply, electricity, and air conditioning, to its automatic feeding machines and smart air filtration and disinfection systems, can be monitored and controlled centrally from a NASA-like command center on the first floor. A stupendous amount of pig manure is processed daily in a biogas-driven waste treatment system and turned into electricity for lighting and heating the buildings. About 400 such ‘pig-rises’ could meet a part of China’s and the world’s growing appetite for animal proteins.
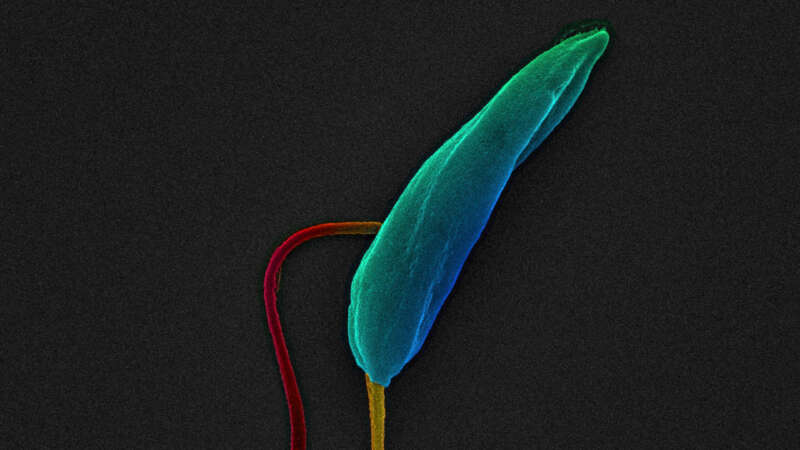
Sand Flies: The Silent Biters Spreading A Deadly Disease
Phlebotomine sand flies are notorious biters. They not only cause great irritation but are also capable of spreading a deadly disease – visceral leishmaniasis.
While the World Health Organization states that currently 1 billion people live in areas endemic for leishmaniasis and at risk of contracting the disease, a recent study using a statistical model, predicted that visceral leishmaniasis (VL) is undergoing geographic expansion and 5.3 billion people could be at risk of acquiring the disease in the future.
Leishmaniasis currently occurs in approximately 90 countries. These countries are located in the warmer climates where sand flies thrive: in the tropics, subtropics, and in Southern Europe. Climate change and other variations in the environment have the potential to expand the geographical range of where sand flies can live and therefore where the disease can infiltrate the human population.
Creating Drug-Free Communities
The Drug-Free Communities (DFC) Support Program is administered by the White House Office of National Drug Control Policy (ONDCP) and managed by the Centers for Disease Control and Prevention (CDC).
The CDC says maternal mortality rates in the U.S. got better, after a pandemic spike
After spiking in 2021, the maternal mortality rate in the U.S. improved significantly the following year, according to a new report from the Centers for Disease Control and Prevention.
The data shows that 817 women died of maternal causes in the U.S. in 2022, compared to 1,205 in 2021. These are deaths that take place during pregnancy or within 42 days following delivery, according to the World Health Organization, “from any cause related to or aggravated by the pregnancy or its management, but not from accidental or incidental causes.”
“I think that the bump [in 2021] reflects the pandemic and we’re returning to pre-pandemic levels,” says study author Donna Hoyert, who a health scientist at the CDC’s National Center for Health Statistics.
Shrinking Forests, Emerging Diseases
Dona Dora’s man is away from home a lot more these days. It didn’t used to be like that.
He leaves early, sometimes on foot, but increasingly on his bicycle, and heads into the forests surrounding Belém, the capital of Brazil’s Para province. He keeps his eyes open especially for five medicinal plants that are always in demand — sucuúba (Himatanthus sucuuba), copaíba (Copaifera spp.), andiroba (Carapa guianensis), barbatimão (Stryphnodendron spp.) and pãu d’arco (Tabebuia avellanedae).
Fifteen years earlier, he would have found all five within hours and been back for lunch, but times have changed. These days, medicinal forest plants in high demand are becoming harder to find as forests that have stood strong for millennia are cleared to make way for grazing pastures for millions of cattle, agriculture, and development.
Now, Dona Dora’s man can spend a whole day and not find more than a few plants. It might be late at night before he gets back home.
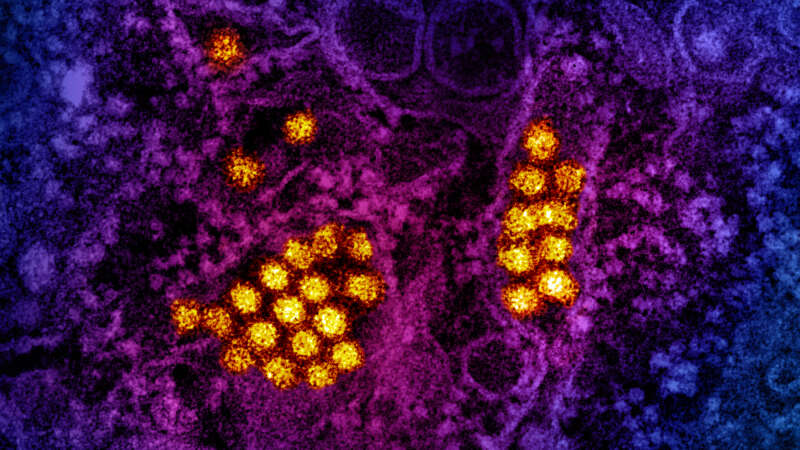
The Rise of Dengue: A Global Perspective
Around the world, dengue is considered the most common viral disease transmitted by mosquitoes that affects people. According to the World Health Organization (WHO), the disease is now endemic in more than 100 countries. In the first three months of 2024, over five million dengue cases and over 2000 dengue-related deaths were reported globally. The figures so far project that 2024 could be even worse than 2023, with the regions most seriously affected being the Americas, South-East Asia, and Western Pacific.
In the Americas, there were 6,186,805 suspected cases of dengue reported in the first 15 weeks of 2024. To put this into perspective, according to the Pan American Health Organization (PAHO), this figure represents an increase of 254% compared to the same period in 2023. Of these cases 5,928 were confirmed and classified as severe dengue.
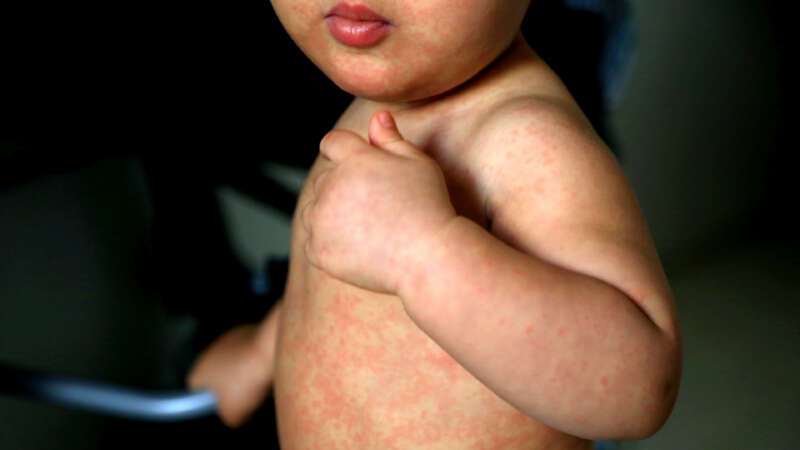
Europe and the U.S. Battle Measles – Again
Initially, doctors in the Tuzla Canton of the Federation of Bosnia and Herzegovina thought the rash on young Imran’s* stomach could be scarlet fever. Or maybe it was Kawasaki disease. As reported by Eurosurveillance, that was in early December 2023. By Christmas, four of Imran’s preschool classmates had been admitted to the hospital with measles. By mid-January 2024, another epidemiologically linked case – again originally misdiagnosed as the much less contagious scarlet fever – presented in a neighboring canton. Two more quickly followed. Between the last week of December and the middle of February, the Balkan nation had reported 141 new measles cases.
Barts Health Trust’s Dr. David Harrington said the misdiagnoses should not be unexpected.
“Many front-line clinicians won’t have seen measles for several years,” he told Medscape UK. “So good education and training and collaboration between public health and infection specialists with those in primary and emergency care is key.”
Mosquitoes that carry West Nile are becoming resistant to insecticides
John VanDenBerg suspects he was gardening when a mosquito got him.
It was September 2018, and VanDenBerg, then 67, had been feeling a little “off” for a few days, he said, like maybe he had the flu.
But one morning, as he was walking out of his Colorado home, he collapsed.
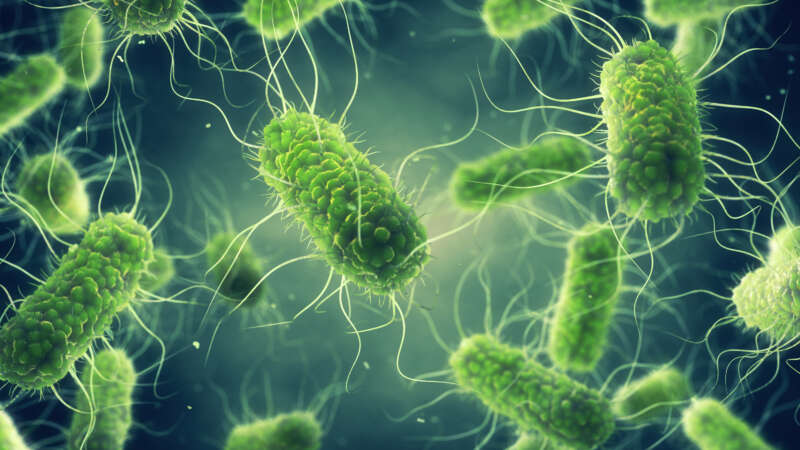
Beyond Salmonella: Emerging Foodborne Threats
Walkerton, a serene town in Bruce County, Ontario, with a population of under 5,000, embodies tranquil rural charm, where close-knit communities thrive amid picturesque landscapes. Here on May 15, 2000, the local public utilities commission took a routine sample of the water supply and discovered E. coli contamination. The commission didn’t notify public health officials.
In the following days, several people fell ill with bloody diarrhea. The local public utilities commission reassured officials a couple of times that the water supply was safe, even though cases kept rising. By the time health officials finally warned the community against consuming untreated tap water, over 40 individuals had already sought medical attention at the hospital.
The Walkerton E. coli outbreak that saw 2,300 people fall ill, and seven die, was the worst public health disaster involving municipal water in Canadian history.
Deforestation’s Hidden Toll: Amplifying Disease Risk Worldwide
In the last couple of decades, the lush rainforest around the remote village of Meliandou in the heart of Guinea has become patchier. Animals, like bats, saw their habitats dwindle and in a quest for survival, they sought refuge in closer proximity to human environments, making the boundaries between species thinner. A hollowed-out tree in the middle of the village became home to a colony of bats.
About 50 meters from the same tree, in the heart of Meliandou, a two-year-old boy named Emile lived with his family. In a matter of days, Emile fell ill with an unknown virus, developed a high fever, and died. Soon the same virus, that scientists now believe Emile got from the bats, took the lives of his sister, mother, and grandmother. The village, surrounded by a ring of forest, unexpectedly became the epicenter of a devastating outbreak that would leave an indelible mark.